Hantavirus Horror: Zimbabwe’s Health Scare – Was the Public Told the WHOLE Truth?
HARARE – Zimbabwe recently found itself at the centre of a significant health concern following the repatriation of three healthcare workers from Ascension Island. The individuals were brought back to the country due to suspected contact with the deadly hantavirus, an event that sparked considerable public anxiety and calls for immediate transparency from health authorities. However, the government’s swift response, epitomised by the Herald’s emphatic declaration, “NO HANTAVIRUS CASE IN ZIMBABWE: GOVT,” has, for some, inadvertently raised more questions than it answered, fuelling speculation about the completeness of the information being shared with the public.
The incident, which unfolded this month, saw the three Zimbabwean health workers arrive in Harare last night. They were promptly placed in quarantine as a precautionary measure, in strict adherence to public health protocols. The Minister of Health and Child Care, Douglas Mombeshora, confirmed these details during a media briefing in Harare. While the government maintained that surveillance and monitoring systems were on high alert, no confirmed cases of the virus had been detected within Zimbabwe’s borders at the time of the announcement.
This rapid denial, while undoubtedly aimed at reassuring a potentially panicking populace, highlights the delicate balance between effective public health communication and managing public perception. In a context where public trust in official narratives can be fragile, such absolute statements can sometimes lead to increased scrutiny rather than outright acceptance. The public remains keen to understand the specifics of the health workers’ exposure, the nature of any symptoms they might have exhibited, and the thoroughness of the investigations conducted on Ascension Island and upon their return.
Understanding the Hantavirus Threat
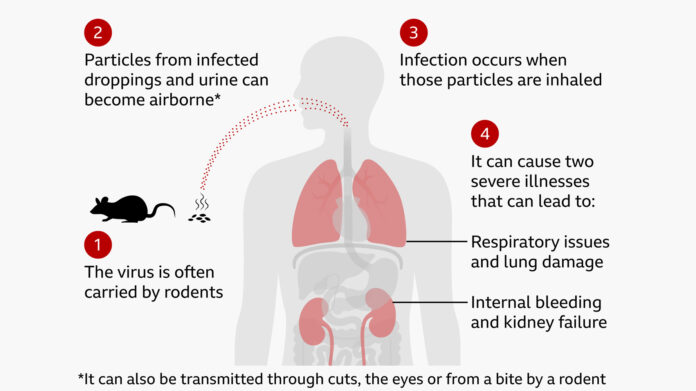
To fully grasp the gravity of the situation, it is crucial to understand what hantavirus is and the threat it poses. Hantaviruses are a group of zoonotic viruses, meaning they are primarily transmitted from animals to humans. Rodents, particularly mice and rats, serve as the natural reservoirs for these viruses. Humans typically become infected through contact with infected rodents or their urine, droppings, or saliva. Less commonly, infection can occur through rodent bites. Activities that increase exposure risk include cleaning enclosed or poorly ventilated spaces, farming, forestry work, and sleeping in rodent-infested dwellings.
Infection with hantaviruses can lead to a range of severe illnesses, often with fatal outcomes. The specific disease manifestation varies depending on the type of virus and geographical location. In the Americas, hantaviruses can cause Hantavirus Cardiopulmonary Syndrome (HCPS), a severe respiratory illness that rapidly progresses and affects the lungs and heart. HCPS is particularly concerning due to its high case fatality rate, which can be as high as 50 per cent. A notable strain, the Andes virus, found in South America, is one of the few hantaviruses for which limited human-to-human transmission has been documented, typically occurring among close contacts during the early phase of illness.
Conversely, in Europe and Asia, hantaviruses are known to cause Haemorrhagic Fever with Renal Syndrome (HFRS), which primarily impacts the kidneys and blood vessels. While still serious, HFRS generally has a lower case fatality rate, ranging from 1 to 15 per cent. Globally, hantavirus infections are relatively uncommon, with estimates suggesting between 10,000 and over 100,000 infections annually. The largest burden of cases is observed in Asia and Europe, with East Asia, particularly China and the Republic of Korea, reporting thousands of HFRS cases each year, although incidence has declined in recent decades. In the Americas, HCPS cases are rarer, numbering in the hundreds annually, but their high fatality rate makes them a significant public health concern.
Symptoms in humans usually manifest between one and eight weeks after exposure. Initial symptoms often include fever, headache, muscle aches, and gastrointestinal issues such as abdominal pain, nausea, or vomiting. In HCPS, these symptoms can quickly escalate to a cough, shortness of breath, fluid accumulation in the lungs, and shock. For HFRS, later stages may involve low blood pressure, bleeding disorders, and kidney failure. Early diagnosis is challenging due to the non-specific nature of initial symptoms, which can mimic other common febrile or respiratory illnesses like influenza, COVID-19, or viral pneumonia. Therefore, a detailed patient history, focusing on potential rodent exposure, occupational risks, travel history, and contact with known cases, is crucial for accurate diagnosis.
There is currently no specific antiviral treatment or vaccine available for hantavirus infection. Treatment is supportive, focusing on close clinical monitoring and managing respiratory, cardiac, and kidney complications. Early access to intensive care significantly improves outcomes, especially for HCPS patients. Prevention strategies primarily revolve around reducing human contact with rodents. This includes maintaining clean homes and workplaces, sealing entry points for rodents into buildings, securely storing food, and practising safe cleaning methods in areas contaminated by rodents, such as dampening surfaces before cleaning to avoid aerosolising viral particles.
Hantavirus vs. COVID-19: A Lethality Comparison
The emergence of any new viral threat inevitably draws comparisons to the recent global experience with COVID-19. While both are viral diseases, hantavirus and COVID-19 differ significantly in their transmission dynamics and lethality. Hantavirus, particularly the HCPS-causing strains, boasts a considerably higher mortality rate. For instance, the Andes hantavirus can have a mortality rate of up to 39.8 per cent, and HCPS generally ranges from 20 to 50 per cent. In stark contrast, the mortality rate for COVID-19 in the United States, for example, was approximately 1 per cent. This makes hantavirus substantially deadlier on a per-case basis.
However, the key difference lies in transmissibility. COVID-19, caused by SARS-CoV-2, is highly contagious and primarily spreads through airborne transmission, leading to its rapid global spread and pandemic status. Hantavirus, on the other hand, is not easily transmitted from person to person. Human-to-human transmission is rare and has only been definitively documented for the Andes virus strain, requiring close and prolonged contact, typically within households. This limited transmissibility means hantavirus has a much lower potential to cause a widespread pandemic compared to COVID-19, despite its higher individual lethality.
South Africa’s Hantavirus Situation and Regional Implications
The hantavirus scare in Zimbabwe takes on added significance when viewed in the context of developments in neighbouring South Africa. In early May 2026, South Africa confirmed a hantavirus-related death, that of a 70-year-old male. This case was linked to the MV Hondius, a cruise ship that has been associated with a multi-country hantavirus cluster. As of May 8, the World Health Organisation (WHO) reported a total of eight cases, including three deaths, linked to this cruise ship cluster, with a case fatality ratio of approximately 38 per cent.
Following the confirmed case, South African health authorities, under the guidance of Health Minister Dr. Aaron Motsoaledi, initiated extensive contact tracing efforts. Of the 97 contacts identified, 90 individuals were successfully traced, with 86 located in Gauteng and four in the Western Cape. Dr. Motsoaledi has been working closely with the WHO to manage the situation and has urged the public to remain calm, emphasising the rarity of human-to-human transmission. The incident underscores the vigilance required even for diseases with limited transmissibility, especially in a globally interconnected world.
The proximity of Zimbabwe to South Africa, coupled with their significant economic ties, raises concerns about potential cross-border transmission. The Beitbridge border post, which connects the two nations, is renowned as the busiest land border in Africa. It facilitates an immense volume of trade and human movement, including a large number of truckers and informal cross-border traders. In 2020 and 2021, for instance, South Africa’s exports to Zimbabwe through Beitbridge amounted to nearly 3.3 billion pieces of goods. This high level of interaction creates a conduit for the potential spread of infectious diseases, as was starkly demonstrated during the COVID-19 pandemic in 2020.
Should hantavirus become more prevalent in South Africa, the risk to Zimbabwe would be considerable, irrespective of the current official denial of local cases. The constant flow of people and goods across the Beitbridge border means that any health crisis in one nation can quickly spill over into the other. This interconnectedness necessitates robust regional health surveillance and collaborative response mechanisms to mitigate the risks posed by emerging infectious diseases.
The Quest for Truth and Transparency
The Zimbabwean government’s assertion that there are “NO HANTAVIRUS CASE IN ZIMBABWE” is a critical statement, yet it exists alongside the undeniable fact of repatriated healthcare workers due to suspected contact. This juxtaposition naturally leads to public questioning. Was the government’s denial based on conclusive, exhaustive evidence from comprehensive testing of the repatriated individuals, or was it a pre-emptive measure designed to prevent public panic, perhaps before all facts were fully ascertained?